The work of helping has never really belonged to a single professional. It has prevailed across centuries in instances of talks exchanged between two family members, in the shared tea between neighbors after a loss, in the voices of a teacher who sees potential long before a student ever does. People have referred to it by various names over time, including counseling, mentoring, consulting, coaching, opinion, advice-giving, etc. However, the essence has remained strikingly similar to that of one human being trying to understand another.
However, today’s world has evolved. Clients no longer approach with a single question or a simple requirement. They arrive with their complete life. An employee who has been unlawfully terminated arrives in a lawyer’s office holding emails and notices, but beneath the documentation lies a nervous system worn down by insomniac nights and piling dread. The psychological disbelief is as genuine as the legal injustice. The most powerful brief in the world will fall flat if the individual opposite does not even feel safe enough to participate in their own defense. Similarly, a victim of domestic violence seeks police protection and legal remedies, but her voice trembles and fractures before she can provide a clear timeline for the FIR. The law requires precise facts, and trauma triggers them in uncontrollable flashes when relived again and again through recounting. In such cases, the most appropriate way to deal is to make legal advocacy and psychological support work together. When they do, she can avoid the impossible choice between evidence accuracy and emotional survival. And this is why the stakes of professional practice today are different from what they used to be. This is especially true about fields whose very foundation relies on human experiences. Degrees may decorate the walls, and polished professional arguments may decorate a professional’s resume, but the real test begins the moment another human being sits across, hoping to be understood. They are all about the fit now. It is not simply whether the professional can help, but whether they are the right kind of help that is needed by the client, and whether they know when collaboration of practices is essential. Professionals have been collaborating long before anyone called it “collaboration.” Doctors have referred patients to specialists for generations. Counselors have worked with psychiatrists when medication became part of healing. Legal advocates have worked with shelters and psychologists to support survivors. These collaborations were never ideological in nature. They were very instinctive responses which highlighted that no single profession can hold the whole of the human experience. Yet professional silos persist in modern times. Therefore, the purpose of this text is to make responsible collaborative efforts accessible to people. Client screening, management, and professional conduct need to be considered in-depth for forming the ethical spine of helping people. These procedures protect the client as well as the practitioner/professional. Such a collaborative, integrative approach deepens the process by providing flexibility, competence, confidence, and care without overreaching the boundaries.
The Historical Evolution of Seeking Guidance
Long before professional institutions existed, human beings sought guidance in the intimate circles of their daily lives. Wisdom, advice, and opinions were all imparted in the spaces of the kitchen, farms, courtyards, and living rooms. They were delivered by community anchors, such as elders or family patriarchs, and were often based on an unwritten social contract where trust was the currency and reputation was the only form of accountability. In this era, support was less about objective science and more about the transmission of personal views.
As society evolved, the shortcomings of this informal system became evident. While guidance was often given with love, it lacked the necessary safeguards, which sometimes led to harmful outcomes such as encouraging endurance in abusive relationships or overlooking trauma. This gap led to the emergence of modern helping professions. Unlike the traditional “village” approach, these professions introduced ethical frameworks, competency standards, and boundaries to protect the seeker. This transition from community wisdom to professional practice was not about replacing human support, but about refining it. It moved the focus from simply telling someone how to live based on tradition to empowering them with evidence-based practices and psychological safety.
Counseling over the years
By the late 1990s, conversations around mental health began to emerge in the mainstream. Internationally, the WHO played a key role in shifting mental well-being from closed academic circles to becoming a global discourse, highlighting issues like depression and burnout as major public health concerns. While India was part of this change, the entry of formal counseling into the cultural mindset was not smooth. For decades, emotional concerns were dismissed as weakness, and mental pain was tolerated in silence. When the concept of counseling first appeared, it was viewed as foreign and unnecessary. “Why talk to a stranger when you have family and elders?” Yet, change came quietly. Through global media exposure, urbanization, and field research, the old assumptions began to fracture. Universities launched courses, hospitals hired professionals, and acceptance slowly grew. This eventually legitimized counseling as a dignified form of support.
However, as counseling gained recognition, an unexpected paradox also emerged. The popularity of the field led to a dilution of the term. The language of mental health was borrowed into spaces where it did not belong, such as corporate offices, training institutes, law firms, and sales departments. Professionals untrained in psychological ethics started claiming to provide “guidance,” “crisis handling,” or “support sessions.” In workplaces, coaching and employee onboarding took hold of counseling vocabulary. Corporate coaches began branding performance feedback as “mental wellness interventions,” and onboarding teams reframed orientation check-ins as “emotional adjustment support.” HR managers reimagined themselves to be “workplace counselors” as well. Academic counselors started selling courses under the guise of “career therapy.” Teachers began acting as “grief counselors” to students without trauma training. The list kept expanding. This created a dangerous overlap. Managers directed employees emotionally without grasping concepts like dependency or transference. The onboarding executives probed into personal struggles and teachers offered grief support without any trauma competencies. Even lawyers offered personal counsel beyond legal scope. “Counseling” slowly became a corporate buzzword for soft skills, performance management, or persuasion. Efforts meant for healing were unintentionally repurposed for productivity and retention. As a result, emotional vulnerability landed in the hands of the ill-equipped. The outcome of this led to public confusion where people could no longer distinguish between professional therapy, corporate coaching, structured counseling, self-help advice, and workplace onboarding conversations.
Simultaneously, a cultural contradiction persisted. While therapy was slowly becoming available, suffering in silence was still perceived as a mark of strength. Emotional exhaustion was treated like a badge of honor, with the societal lexicons like “what does not kill you makes you stronger” dominating the collective psyche of Indian society. The fear of social judgment often outweighed personal well-being. Many avoided help to protect their family’s reputation, waiting until a breaking point occurred. Emotional collapse was either normalized or minimized to fit the image of resilience. Thus, even as mental health awareness became trendy, the actual act of seeking help remained shrouded in shame. With this, the helping profession grew more and more complex. This led to a surge for demand and clarity from the profession itself. Advocacy bodies began to insist that emotional support required structured training, evidence-based knowledge, and strict ethics. A credential revolution took place, which aimed to establish clear distinctions that only registered practitioners could now diagnose to provide counseling. This structural reform came at the cost of “siloing” of expertise. Mental health became separated from daily life, forcing the clients to navigate a maze of specialists who rarely communicated with one another. Consequently, the modern client evolved too. No longer passive recipients of advice, they became active participants who scrutinized degrees, reviews, and ethical codes before engaging with the service of the professional. Couple it with the rapidly rising hyper-awareness that has resulted in clients self-diagnosing using online resources to avoid the embarrassment of an initial professional visit. This is a trend that, again, risks misinformation. They were not simply seeking help anymore; they verified expertise, acknowledging that while support is human, professional intervention required specific, trusted competence.
The Case of Collaborative Practice
The history above of formalized counseling shows that professional boundaries (while necessary for competency and client safety) often lead to siloing of human problems. However, the professionals have also somewhat come to terms with the fact that real human problems rarely stay inside neat compartments. A purely legal solution may not heal trauma, or a financial plan may not automatically repair a wounded relationship with money, or therapy sessions alone cannot finalize child custody. When a human being arrives seeking support from a professional for whatever cause, they are probably carrying a whole lot of their life along and not just isolated pieces. Let us consider a case of divorce here.
A divorce case may involve trauma for the child about the child custody decisions and the separation of parents. Lawyers can argue about custody, draft petitions, and build a legal narrative very well. However, they are not equipped to untangle the psychological wounds left by the emotional abuse that the child may have faced. Without the possible involvement of a trauma-informed mental health professional, the court may reach a legally sound verdict, but may never reach one that will emotionally validate the people involved. Similarly, an individual who ends up in a business dispute, losing sleep over the betrayal by a co-founder, may choose to proceed with litigation. On paper, this may seem like a straightforward case of breach of contract. However, in the human heart, it is a blow to trust, self-belief, and identity. The anxiety that builds during litigation shaped negotiation decisions, settlement terms and even the stamina to continue the process. Here, a legal strategy alone cannot support someone whose mental resilience has collapsed under pressure. Cases like these prove that helping a person means seeing the individual as a whole person and not just the part that belongs to just the professional’s discipline.
This calls for the rise of a collaborative approach amongst professions, one that refuses to isolate such processes, which are so deeply layered. Integrative and collaborative practice here does not mean that everyone does everything. No. It means professional work needs to happen in conjunction with others. The client’s life becomes the organizing principle, and not the profession’s boundaries. In such a model, a lawyer handling a high-conflict custody case may recommend that a trauma-informed therapist be involved. This means that the professional acknowledges the emotional and mental state of the client, and simultaneously understands that the client deserves support across domains. Here, collaboration is an act of deepening the expertise by giving the client the open option of engaging with multiple professionals while maintaining their primary need. The lawyers can simultaneously keep the process of custody running while also helping the client connect with a certified professional so that the client is fully prepared to face the process of custody. A professional consults only with the client’s knowledge and consent. They establish appropriate communication protocols to safeguard the confidentiality of the process. Information is shared responsibly to support the client’s well-being so that their privacy is not compromised. Each specialist acts within their domain while acknowledging where another field is essential. The result is continuity of the client’s care rather than fragmentation of their problems.
Such integrated care is not an innovation anymore globally. Multidisciplinary clinics routinely house psychologists, psychiatrists, nutritionists, and legal advisors under one roof. Many law firms in developed nations employ in-house counselors because they understand that high-stakes legal matters may dig up trauma, fear, and grief. Corporate wellness programs in several global companies include financial therapists alongside workplace counselors and HR professionals. India is also catching up; however, not at the pace it should. Cultural hesitations around mental health, infrastructural gaps, and a lack of awareness slow the acceptance of such collaborative models. The peak irony is that every legal notice explicitly mentions “emotional harassment,” “mental agony,’ or “distress caused.” Yet, when the time comes to involve the said mental health professionals, the conversation suddenly turns silent. Emotional suffering is recognized in conversations and papers, but resisted vehemently practically. This further solidifies the call for integration of various services. Because real people live at the crossroads of multiple disciplines every single day. To serve such clients fully and ensure that they receive long-term, sustainable benefit and recovery in their lives, the professions must learn to meet at the intersections, too.
The Core Components
If collaborative care is the most efficient future for professional practice, then it cannot simply rely on goodwill or intuition. Collaboration requires a streamlined structure. A seamless client experience is a result of a deliberate framework that allows multiple professionals to work together without blurring roles, boundaries, or accountability. Integrated practice is a system and that system needs components that will make it dependable. Every profession stands on decades of specialized knowledge obtained with thorough research, ethical codes, and intensive training. Collaboration and integration of various disciplines do not erase that. On the contrary, it honors the boundaries so that each discipline can function at its supreme level. A counselor cannot put on the hat of a legal strategist. Or a lawyer cannot turn into a trauma specialist. True collaboration begins with the ability to admit that every part of the client journey does not rest with the primary professional, and that is precisely why the collaboration matters. In this collaborative framework, boundaries are doors to a seamless client journey. Each professional knows when to enter, when to observe, and when to step back. The client experiences continuity as no one attempts to “replace” another discipline. On a similar note, no one is expected to carry an entire human life alone.
The core of this model is the very idea that the client’s journey is more important than any profession’s identity. Instead of shouldering the entire journey alone, the professional searched for what the client needed the most at the moment. Based on that, they can make appropriate suggestions for what needs to be done in the client journey next and, if necessary, which professional they can connect their client to for a smoother journey. Collaboration then unfolds as a fluid sequence based on the client’s evolving conditions. The client may begin in one professional’s office, which can be the primary professional service handling the main pain point of the client. When new information emerges that reveals emotional, relational, or psychological complexities, the primary professional may propose to initiate a structured co-management plan with the client’s consent. If the situation is more aggravated than expected, they may even choose to initiate a structured referral if they deem it fit that the client needs psychological care more than the primary professional service. Each specialist contributed within their domain, and information is shared in a responsible and measured manner. This way, the client may not feel being “passed around.” Instead, they may feel supported in more than one dimension of their life. It makes sure that the support matches the complexities that the human across the table is facing.
The Mechanics of Client Screening and Assessment
Every profession dealing with people eventually arrives at the same realization that it is impossible to offer meaningful help to someone whom you have not first understood. And this process of understanding is a time-consuming task. It is not a miracle, and certainly does not happen automatically. Clients do not walk in and immediately hand over their truth. This is usually because we Indians have been trained for a lifetime to protect parts that hurt. What begins on the surface as paperwork or guidance almost always reveals a much deeper emotional landscape beneath. This is why client management can never be a mechanical sequence. It is a relationship before it becomes a service. The journey of this service begins with the screening of the client, as well as the simultaneous rapport formation that happens.
The first interaction determines whether the client feels judged, minimized, or genuinely seen. Rapport becomes a strategy that allows the client to show their real experience without the fear of consequence. Carl Rogers described empathy, unconditional positive regard, and congruence as the core conditions for effective helping. In India, these conditions take on an even deeper dimension as trust is earned through warmth, patience, and respect for the realities lived by the families, their culture, community, and social expectations. Indian clients often arrive with hesitation. This is partly because they have been conditioned to downplay their pain. A woman going through a messy divorce may say that she is alright, even as her trembling fingers may betray her words. In such moments, rapport is formed by how deeply the professional listens to the client. The path of rapport with hesitant clients can often be observed as a process that moves through gentle, incremental steps, slowly guiding the client to warm up to the professional and their team. This rapport goes through ebbs and flows throughout a case and requires constant reinforcement. When trust is ever-present, the client will tell exactly who they are. However, when it is missing, the client will tell who they think they are supposed to be.
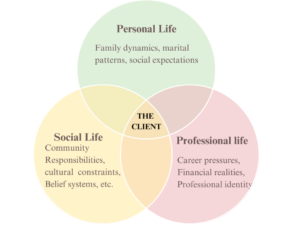
Screening looks for the person with the problem. This requires special sensitivity, especially in India, where people often speak in coded language due to emotional, cultural or unconscious reasons. A man involved in a property dispute may insist that he is sleeping well while constantly fidgeting with his fingers. A middle-aged woman attending mediation may laugh too loudly to mask the terror of yet another confrontation with her abusive spouse. None of these clients is trying to deceive the professional. They are simply trying to survive. Screening, therefore, is not the very observation of the human being sitting across from us. It studies the timeline of events, along with the emotional reactions. It listens to the words along with the silences. It respects the stories while simultaneously noticing the gaps the client did not consciously intend to leave. A man may suddenly skip over the details surrounding the legal notice being served or a woman may jump to the settlement discussion while avoiding every detail of the marriage. This is where the essence of screening becomes all the more visible. At the same time, screening serves the functional role of determining whether the professional’s services are appropriate, identifying the client’s goals on deep levels of emotions, evaluating the readiness for change, exploring risk factors like self-harm, trauma or substance use, and laying the foundation for the service planning. And it begins much earlier than the formal assessment. The tone of the initial phone call, the wording of the first email, and the seating arrangement during the intake are a few of the things that can contribute to whether the client feels safe enough to speak truthfully. A well-conducted intake interview balances the structure. It gathers history while making space for emotions. It guides the discussion gently without overpowering the client’s rhythm for disclosure. Most importantly, it adapts to the person and not the other way around. When screening holds the capacity to evolve into a multi-dimensional assessment, the professional begins to understand the entire ecosystem on which the client sustains. This can include their family dynamics, career pressure, relational patterns, social expectations, community responsibilities, economic realities, and even their spirituality. Clients do not exist inside single problems. They exist inside systems that ultimately shape their behavior far more than isolated events.
Screening and assessment are also often framed as processes to understand the client better, but in reality, this is a two-way street. They also help the professional understand whether they are the right person for this case, whether they have the emotional and technical bandwidth for it, and whether the client is in a state that allows any real work to begin. Just as the client evaluates whether they can trust the professional, the professional evaluates whether the working relationship can be safe, ethical and productive. Through careful screening, professionals often recognise risk long before the client does. A lawyer might realise that a client’s uncontrollable panic or impulsive aggression will make legal decision-making chaotic and dangerous if not addressed first. In such cases, screening protects the clients while also protecting the professional from walking blindly into a situation where their expertise alone cannot keep the process safe. It is normal to get some clients who may be labelled “high-risk.” They may not be typically difficult people to work with, but can also be overwhelmed people. High emotional arousal, untreated paranoia, trauma, extreme anxiety, spiraling guilt, or hopelessness are a few things that can derail any professional process. In such cases, pushing ahead with legal strategy or financial planning or conflict mediation can do more damage than good. There are moments when the most ethical and most competent choice is to pause the work and recommend mental health support before anything else continues. This makes the progress actually possible. Good screening helps the professionals recognise when their emotional state might interfere with the case, allowing them to seek supervision, co-working, or temporary support from another specialist. It keeps the work ethical and healthy. If the professional does not notice a client’s psychological distress early, they might misinterpret behavior. Their withdrawal may look like non-cooperation, panic may look like irrationality, dissociation may look like dishonesty, and trauma may look like stubbornness. Accurate assessment prevents professionals from internalizing these things. It clarifies whether a client is resisting because they are unwilling, or because they are drowning. And this difference changes everything. The way deadlines are set, the tone of the communication, the pace of sessions, whether family involvement is recommended, or whether collaboration with another expert becomes necessary.
The Ethical Framework
When multiple professionals come together for the well-being of one client, ethics is no longer a background document but the backbone of practice. Collaboration can be powerful, but it needs to work on the terms of clarity. The client must know exactly who is involved in their care, what roles each person plays, and how information will move between the professionals. In collaborative practices (especially between two independent professionals), informed consent emerges as an anchor. Explaining the collaborative model clearly, asking for permission before adding team members, and checking whether the client feels ready and safe with the arrangement builds the kind of trust without which no real progress is possible. Confidentiality goes in the same breath when there is more than one professional in the room. Clients need to know what will be shared, why, and with whom. A counselor may share information relevant to a legal case and vice versa, but not the intimate details irrelevant to the legal matter. A lawyer may update a mental health professional about a major hearing date that might trigger anxiety, but has no right to disclose sensitive personal history. In collaborative work, boundaries matter more than they do in solo practice because in collaborative efforts, each professional must stay in their lane, avoid overstepping into another’s territory, and respect the limits of their own training. The absence of such discipline can easily turn collaboration into chaos or worse, unintentional harm.
Collaboration is also a communication question. A legal professional who consults with a counselor should not do so only when a crisis arrives; regular check-ins, shared documents (with client permission), and careful progress updates prevent misinterpretations that could reverse months of progress. A counselor might observe heightened panic that could jeopardise a client’s rational legal decisions. A lawyer might notice self-blame worsening after every court date, needing therapeutic attention. The system works only when communication flows both ways respectfully, concisely, and always with the client at the centre, not the professionals’ egos. Coordination also demands timing. Sometimes the question is not whether collaboration is needed, but when. A counsellor may delay trauma work because the legal case requires immediate cognitive stability. A financial advisor may postpone planning until therapy stabilises compulsive spending tendencies. In well-functioning systems, every professional understands that client autonomy remains the highest authority. Nothing moves without the client’s permission, and nothing is shared because “it might help”. It also helps as an enabling platform for the professionals themselves. The client approves every step. To uphold an integrated model ethically, practitioners must constantly grow. Collaboration requires more than knowledge of one’s own discipline; it requires curiosity about adjacent fields. A lawyer does not need to become a therapist to understand trauma triggers. A counsellor does not need a law degree to understand the emotional impact of custody battles. Continuous education keeps professionals sharp, aware, and humble. Cultural competency and trauma-informed practice are no longer optional luxuries; they are mandatory for anyone working in the landscape of human suffering.
And behind all this is a truth professionals rarely admit aloud: helping people takes a psychological toll. Bearing witness to pain, conflict, loss, and helplessness can wear the strongest minds down. Burnout and compassion fatigue happen because professionals are human. Healthy collaboration includes caring for the caregivers. Peer consultation, supervision, breaks between emotionally heavy cases, and a culture that normalises seeking support instead of glorifying exhaustion are not indulgences; they are part of ethical practice. This two-way street can be accessed by professionals too. They may find it easy to initiate conversation with other relevant professionals as well when the need arises. A lawyer may find or seek help from a counselor for their own personal distress they may have faced while providing services to a client. Similarly, a counselor may seek out the assistance of a lawyer in times of need when they get involved with a risky client. A professional who never refuels eventually becomes unsafe, not because they lack skill, but because they lose their emotional footing.
The Path Forward
For decades, advice-giving, mentoring, and emotional support have sustained countless individuals in India. Friends, relatives, teachers, spiritual leaders, and even strangers have stepped in when someone felt lost. But compassion alone cannot replace competency. When mental, emotional, behavioral, or other difficulties escalate, goodwill alone cannot compensate for the absence of a structured professional support. Modern times have called for an upgrade to casual advice-giving. It is about time to acknowledge that training, supervision, and evidence-based methods protect both clients and the service providers themselves. A formal system ensures that no one has to rely on guesswork when navigating deeply personal struggles. Clients benefit through more accurate screening, ethical safeguards, continuity of care, improved outcomes, and a predictable, reliable process that does not depend on luck, personality, or chance. In short: empathy deserves the support of expertise.
India is standing on the threshold of a cultural shift. The sooner integrated professional services become normalized, the sooner the public will come to expect — and demand — quality, accountability, and collaboration in every form of care. For that shift to occur, awareness cannot remain limited to academic circles or mental-health spaces. Sensitization must reach the mainstream. Schools, workplaces, healthcare systems, and media channels play critical roles in shaping attitudes toward holistic well-being. The taboo around mental health, especially the idea that emotional and psychological struggles must be concealed, needs to be confronted rather than tiptoed around. Every success story must speak loudly. Every example of someone who improved because of timely professional intervention needs space in public memory. When the community stops whispering about struggles and begins speaking openly about recovery, help-seeking automatically becomes stronger, safer, and socially supported. If anyone is considering seeking help, they deserve support that does not fragment their life from another. They deserve an approach that recognizes them as a full, complex human being. No one should have to choose between mental health professionals, career guides, wellness experts, or legal aids when their reality contains all of these dimensions simultaneously. Their well-being deserves a team. Asking for help needs to evolve as a sign of someone who refuses to settle for silent suffering. When choosing a professional, one must look for credibility, transparency, proper credentials, and, most importantly, a willingness to collaborate with other experts when their situation requires more than one lens. The future care is integrative, and globally, it is already a standard. It is time for all of us to catch up and eventually lead the field.








